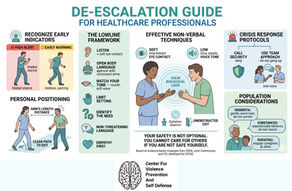
DE-ESCALATION GUIDE FOR HEALTHCARE PROFESSIONALS
- William DeMuth
- 4 hours ago
- 10 min read
Recognizing Pre-Attack Indicators • Verbal & Non-Verbal Techniques
Crisis Intervention • Self-Protection • Post-Incident Care
For life-threatening emergencies, call security or 911 immediately
De-Escalation Guide For Healthcare Professionals Introduction & Purpose
Workplace violence in healthcare settings is alarmingly common. Nurses, physicians, paramedics, mental health workers, and support staff face a disproportionately high risk of verbal abuse, threats, and physical assault compared to nearly any other profession. This guide equips healthcare professionals with evidence-based strategies to recognize danger early, reduce tension effectively, and protect themselves and their colleagues.
This guide is organized around five core principles:
• Early recognition of pre-attack behavioral indicators
• Environmental awareness and personal positioning
• Verbal and non-verbal de-escalation techniques
• Crisis intervention and team response protocols
• Post-incident self-care and reporting

📊 Understanding Workplace Violence in Healthcare
Type | Description | Common Source |
Type I: Criminal Intent | Violence by someone with no relationship to the facility | Robbery, active intruder |
Type II: Patient/Client | Violence from those receiving care; most common in healthcare | Patients, residents, visitors |
Type III: Worker-on-Worker | Harassment or assault between staff members | Colleagues, supervisors |
Type IV: Personal Relationship | Violence from someone with a personal relationship to the employee | Domestic partner, ex-partner |
🔴 Pre-Attack Indicators
Identifying early warning signs is your most powerful tool. Most violent incidents follow a predictable escalation pattern. Learning to recognize these indicators gives you the critical window to intervene before a situation turns physical.
Behavioral Indicators
🔴 HIGH ALERT — Potential Imminent Threat |
• Target glancing — repeatedly looking at you, exits, or security |
• Bladed stance — turning body sideways, dropping one shoulder |
• Clenched jaw, clenched fists, whitening of knuckles |
• Rapid, shallow breathing with visible chest rise |
• Thousand-yard stare or sudden, unnatural calm after agitation |
• Hands hidden behind back, in pockets, or under clothing |
• Invading personal space despite verbal or physical cues to stop |
• Pacing, rocking, or inability to remain still |
• Picking up or handling objects (potential weapons) |
🟠 CAUTION — Escalation Warning Signs |
• Voice volume increasing, pitch rising, speech becoming faster |
• Personal space violations — standing too close |
• Profanity, insults, or derogatory language toward staff |
• Refusing to follow instructions or repeatedly interrupting |
• Pointing or jabbing finger aggressively |
• Expressing hopelessness, stating there is “nothing to lose” |
• Threatening statements even if framed as “just venting” |
• Demanding immediate action with unrealistic expectations |
• History of prior violent or threatening incidents |
🟡 AWARENESS — Early Warning Signs |
• Restlessness, irritability, or low frustration tolerance |
• Emotional lability — rapid mood swings |
• Tearfulness, despondency, or expressions of despair |
• Complaints of being treated unfairly or being singled out |
• Excessive demands on staff time or attention |
• Refusal to engage in conversation or make eye contact |
• Pacing or repeatedly leaving and re-entering the area |
• Signs of intoxication, altered mental status, or acute psychosis |
Physical & Physiological Indicators
The human body telegraphs aggressive intent through involuntary physiological responses. Watch for:
Physiological Signs | Posture & Micro-expressions |
Flushing of the face and neck | Sudden pallor (going very pale) |
Visible perspiration on forehead or hands | Dry mouth — repeated swallowing or lip licking |
Dilated pupils or wide, staring eyes | Muscle tension in the neck and shoulders |
Trembling hands or body | Rigid or stiff body posture |
Exaggerated startle response | Micro-expressions of rage, contempt, or fear |
Hyperventilation | Sudden, inappropriate calmness |
Situational Risk Factors
Certain environments and circumstances significantly elevate risk. Be especially vigilant when:
• Working alone, especially during night shifts or in isolated areas
• Triaging or treating patients under the influence of substances
• Dealing with long wait times, overcrowding, or perceived neglect
• Informing patients/families of bad news, death, or serious diagnoses
• Treating involuntary holds (5150, 302) or forensic patients
• Entering patient rooms alone, particularly with psychiatric patients
• Visitor tensions are elevated (family conflict, grief, disagreement over care)
• Working in high-risk departments: ED, psychiatric units, ICU, oncology, addiction treatment
🏛️ Environmental Awareness & Positioning
Know Your Environment
Always identify exits before beginning any patient interaction
Position yourself between the patient and the door - never let the patient block your exit
Maintain at least one arm’s length distance (6–8 feet) when tension is present
Do not enter enclosed spaces (medication rooms, supply closets) with an agitated individual
Keep furniture between yourself and the patient if tension is rising
Be aware of potential improvised weapons: IV poles, chairs, trays, syringes
Personal Safety Positioning
✅ DO | ❌ AVOID |
Stand at a 45° angle, not directly facing the person | Standing face-to-face in a confrontational stance |
Keep hands visible and relaxed at your sides | Crossing arms, putting hands in pockets |
Maintain clear path to exit behind you | Letting patient get between you and the door |
Keep personal space of 3–6 feet | Moving into the patient’s immediate space |
Wear ID badge on breakaway lanyard | Wearing loose scarves or lanyards that can be grabbed |
Remove or tuck away dangling jewelry | Wearing earrings or accessories that can be pulled |
🗣️ Verbal De-Escalation Techniques
Verbal de-escalation is a structured communication approach aimed at reducing emotional arousal and moving the individual from reactive to rational thinking. The goal is not to “win” the interaction but to establish safety.
The LOWLINE Framework
Letter | Stands For | What It Means in Practice |
L | Listen | Give full, undivided attention. Do not interrupt. Nod to signal understanding. |
O | Open Body Language | Uncross arms, face slightly sideways, keep hands visible and relaxed. |
W | Watch Your Tone | Speak slowly, softly, and evenly. A calm voice is biologically calming to the listener. |
L | Limit Setting | State clear, simple expectations calmly. “I need you to lower your voice so I can help you.” |
I | Identify the Need | Ask what they need or fear. Validate the emotion behind the behavior. |
N | Non-Threatening Language | Avoid commands, ultimatums, and jargon. Use “I” statements over “you” statements. |
E | Empathy First | Acknowledge their distress before problem-solving. “I can see this is very frightening.” |
Effective Verbal Strategies
Validating Responses
• “I can hear how frustrated you are. Let me see what I can do.”
• “You have every right to feel upset about this. Let’s work through it together.”
• “I understand waiting this long is incredibly difficult. I appreciate your patience.”
• “I’m sorry this happened to you. You deserve answers.”
Redirecting Responses
• “Let’s focus on what we can do right now to make things better.”
• “I want to help you. Can you help me understand what you need most right now?”
• “Is there someone I can call for you- family or a support person?”
• “Let’s step somewhere quieter so we can talk without interruption.”
Limit-Setting Responses (Delivered Calmly, Once)
• “I need you to lower your voice so I can focus on helping you.”
• “I’m happy to keep talking, but I need us both to remain calm.”
• “If this continues, I’ll need to involve the charge nurse/security.”
• “Your safety matters to me. Right now I’m concerned about what I’m seeing.”
Language to Avoid
Avoid This Language | Instead, Try This |
“Calm down” | “I hear how upset you are- let me help” |
“You need to…” | “What would help most right now?” |
“That’s not my problem” | “Let me find the right person to address that” |
“I don’t know what you want me to do” | “Tell me what matters most to you” |
“There’s nothing I can do” | “Let’s look at what options we do have” |
Threatening ultimatums | Clear, calm expectations set once |
Sarcasm or dismissive humor | Genuine, warm tone |
Arguing about facts during acute agitation | Validate first; facts can come later |
🤝 Non-Verbal De-Escalation
Studies show that up to 70–93% of communication is non-verbal. Your body language either reinforces or undermines your words. In high-tension situations, non-verbal signals are processed first.
Element | ✅ Calming Approach | ❌ Escalating Approach |
Eye Contact | Soft, intermittent eye contact; look away periodically | Prolonged, intense staring or complete avoidance |
Facial Expression | Neutral to warm; slight nod, soft brow | Frowning, eye-rolling, raised eyebrow, tight jaw |
Voice Tone | Low, slow, steady, and even | High-pitched, fast, sharp, or clipped |
Gestures | Open palms, slow movements, hands visible | Pointing, jabbing, sudden gestures |
Proximity | 6–8 feet; respect cultural norms | Entering personal space uninvited |
Posture | Relaxed, slightly turned, non-threatening | Arms crossed, hands on hips, leaning in |
Movement | Slow, deliberate, predictable | Sudden, quick, or erratic movement |
Breathing | Visibly slow and steady (models calm) | Rapid or held breath (signals tension) |
🚨 De-Escalation Guide For Healthcare Professionals - Crisis Response Protocols
Step-by-Step Response Framework
Step | Action | Key Points |
1 | Assess the Situation | Quickly gauge: Is there an immediate threat? Is a weapon involved? Am I safe to proceed? |
2 | Call for Backup Early | Do not wait for escalation. Notify security or colleagues using code language or panic alarm before you feel unsafe. |
3 | Ensure Your Safety | Ensure your exit path is clear. Move toward the door if safe to do so without provoking the individual. |
4 | Engage Calmly | Speak slowly. Acknowledge the person. Use their name if known. “Hello, I’m [name]. I’m here to help.” |
5 | Listen Actively | Allow them to speak without interruption. Avoid defensiveness. Reflect back what you hear. |
6 | Validate & Redirect | Acknowledge their distress, then move toward solution-focused conversation. |
7 | Set Limits (If Needed) | Calmly state expectations once. Do not repeat it like a threat. |
8 | Disengage Safely | If de-escalation fails, create distance, call for help, and do not pursue. |
Team-Based Response (Code White / Aggression Protocol)
Know your facility’s specific code system. A coordinated team response is significantly safer and more effective than individual intervention.
Designate a primary communicator - one calm voice only; multiple voices increase agitation
Others should position around the perimeter, not crowding the individual
Remove other patients and bystanders from the immediate area
Have security ready but not immediately visible unless the threat is active
Debrief immediately after every incident - brief, factual, supportive
When to Call Security or 911 Immediately
🔴 CALL FOR HELP NOW - Do Not Attempt to De-escalate Alone |
• A weapon is visible or suspected |
• Physical assault has occurred or is imminent |
• Threats are specific, credible, and directed at staff or patients |
• The individual is actively psychotic and not responding to voice |
• You feel unsafe for any reason - trust your instincts |
• The person is blocking exits or restricting movement of others |
• Intoxication is severe and the person is highly agitated |
🧠 Special Considerations by Population
Mental Health & Psychiatric Patients
Use short, simple sentences - complex language increases confusion and agitation
Do not argue with delusions or hallucinations; acknowledge their experience without validating false beliefs
Reduce environmental stimulation: dim lights if possible, reduce noise
Avoid sudden movements or unexpected touch
Offer choices to restore a sense of control: “Would you prefer to sit here or over there?”
Patients Under the Influence of Substances
Expect unpredictable behavior; the standard escalation model may not apply
Speak slowly and repeat key points - impairment affects processing speed
Avoid reasoning or negotiating; focus on safety and simple redirection
Do not leave the person unmonitored in an unsecured area
Request medical evaluation for dual management of intoxication and agitation
Dementia & Cognitive Impairment
Approach from the front; never startle from behind or the side
Use a gentle, warm tone and facial expression - emotion is processed before words
Avoid confrontation, correction, or reality orientation during acute agitation
Use distraction and redirection: familiar music, a preferred object, or a calm environment
Investigate underlying causes: pain, infection, hunger, overstimulation
Pediatric Patients & Families
Engage parents and caregivers as allies, not adversaries
Use developmentally appropriate language with children
Acknowledge parental fear - it is the primary driver of aggressive family behavior in pediatric settings
Ensure consistency in communication: conflicting messages from staff increase family distress
💚 Self-Care & Post-Incident Support
Immediate Post-Incident Steps
• Remove yourself from the situation as soon as it is safe to do so
• Report every incident - verbal threats and intimidation included
• Complete incident documentation while details are fresh
• Seek medical evaluation if physically harmed
• Request a debrief with your team or supervisor
• Accept support from colleagues; do not isolate
Recognizing Acute Stress Reactions
It is normal to experience a range of responses after a frightening incident. These may include:
• Shakiness, nausea, rapid heart rate immediately after
• Intrusive thoughts or replaying the event
• Difficulty concentrating or sleeping in the days that follow
• Hypervigilance or feeling on edge at work
• Irritability, emotional numbness, or withdrawal
Self Care Resources
These are normal stress responses. They typically resolve within days to weeks. Seek professional support if symptoms persist beyond two to four weeks or significantly impact your functioning.
Building Long-Term Resilience
Individual Strategies | Organizational Support |
Regular clinical supervision | Annual de-escalation and safety training |
Peer support programs | Adequate staffing ratios |
Employee Assistance Programs (EAP) | Physical safety upgrades (duress alarms, panic buttons) |
Mindfulness & stress reduction practice | Zero-tolerance institutional policy |
Clear reporting culture with management support | Access to trauma-informed counseling |
📋 De-Escalation Guide For Healthcare Professionals Quick Reference Summary
🔴 PRE-ATTACK: Watch For These Immediately |
• Bladed stance, clenched fists, hidden hands |
• Thousand-yard stare or sudden unnatural calm |
• Target glancing at you or exits |
• Statements of hopelessness or “nothing to lose” |
• Picking up objects that could be used as weapons |
🟠 DE-ESCALATION: Key Principles |
• One calm voice only - never gang up or crowd |
• Validate emotion before correcting behavior |
• Give choices to restore a sense of control |
• Speak slowly - your calm is contagious |
• Position yourself near an exit at all times |
• Call for help early, before you feel unsafe |
🟢 POST-INCIDENT: Non-Negotiable Steps |
• Report every incident, including verbal threats |
• Complete documentation immediately |
• Seek a debrief and peer support |
• Access EAP or counseling if symptoms persist |
• Advocate for systemic safety improvements |
📚 De-Escalation Guide For Healthcare Professionals References & Further Resources
This guide draws on evidence-based frameworks from the following organizations and literature:
• The Joint Commission: Sentinel Event Alert on Physical and Verbal Violence Against Health Care Workers
• Occupational Safety and Health Administration (OSHA): Guidelines for Preventing Workplace Violence for Healthcare and Social Service Workers
• Crisis Prevention Institute (CPI): Nonviolent Crisis Intervention® Training Program
• American Nurses Association (ANA): Reporting Incidents of Workplace Violence
• National Institute for Occupational Safety and Health (NIOSH): Violence in the Workplace
• Emergency Nurses Association (ENA): Position Statement on Violence in the Emergency Care Setting
For facility-specific protocols, duress alarm systems, and EAP resources, consult your department manager, human resources, or occupational health team.
This guide should be reviewed and updated annually in collaboration with clinical leadership and security.
Your safety is not optional. You cannot care for others if you are not safe yourself.